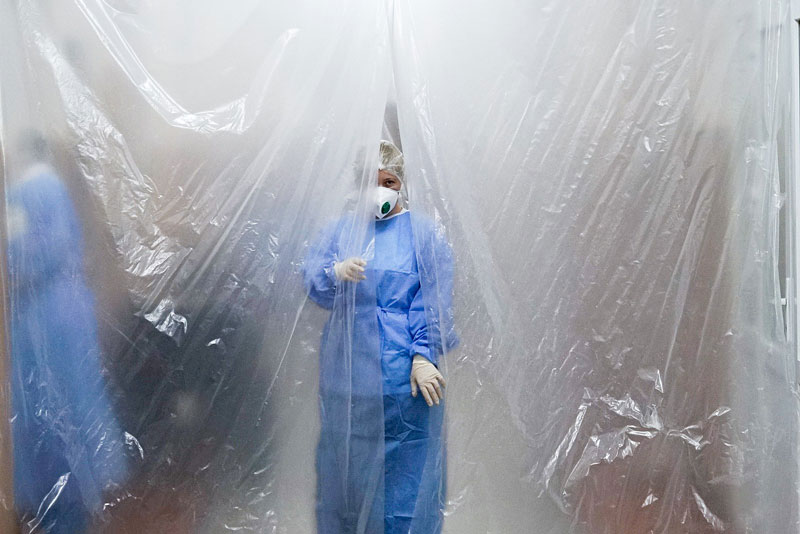
An ongoing study in Ontario is shedding light on how COVID-19 restrictions are impacting the quality of life of seniors and veterans in long-term care homes and their caregivers.
This data will help managers and policy-makers during future pandemics and disease outbreaks, said Annie Robitaille, who holds the research chair on frailty care at Perley Health in Ottawa (formerly the Perley and Rideau Veterans’ Health Centre).
The research is not solely based at Perley Health, which is home to more than 600 seniors and veterans in long-term care. Research is being conducted at seven long-term care homes in order to illuminate the effects of different decisions and practices during the COVID-19 crisis on residents’ quality of life as well as the impacts on caregivers. The research has received financial support from the Legion National Foundation.
By November, weekly interviews had been conducted with 43 caregivers over a five-month period to track how changes affected residents and caregivers.
Preliminary results show caregivers carried a huge burden of guilt during the pandemic about “keeping their loved ones in long-term care, not knowing how they’re doing and not being able to see them,” said Robitaille.
Restrictions greatly complicated caregiving.
Sometimes visits were not allowed, other times homes restricted the number of caregivers allowed in, making it difficult for families who work in teams to provide care for loved ones. Some had to choose which person would be designated, and “when responsibility falls on one individual, the emotional burden becomes a factor,” said Robitaille.
Families greatly appreciated flexibility, the “many times staff understood some of the challenges faced by families and their loved ones.” Those challenges included allowing family members to briefly remove their masks or move temporarily closer so residents could recognize them.
Though it is too early in the process for recommendations, said Robitaille, who stressed that these are preliminary results, there are several commonalities among caregivers.
First, technology to keep residents in touch with family caregivers “worked nicely for some people, but not for everyone.”
Secondly, “a lot of caregivers felt government was to blame for decisions and restrictions, rather than long-term care homes and staff,” said Robitaille. Respondents felt much more needed to be done to prioritize quality of life while observing safety and security measures.
“A long-term care home definitely needs to be viewed as someone’s home,” said Robitaille. “[Residents] can and should be able to make choices with regard to their own lives.”
The next step in the process is to interview seniors and veterans who live in the long-term care centres and the volunteers and staff who work there. Results of the study were to be available early in 2022.

disinfects common areas of a nursing home [wikimedia.org]
Advertisement